Correction of chest wall anomalies, once avoided because of the scope of surgery, is now standard care.
In the not-so-distant past, children born with deformities of the chest wall frequently were resigned to live with their conditions. The most common of these include pectus excavatum and pectus cavernatum; people born with pectus excavatum (PE) bear a telltale sunken chest caused by abnormal curvature of the ribs toward the spine, while those with pectus cavernatum (PC) have the opposite problem, a bulging of the chest caused by malformed ribs protruding outward.
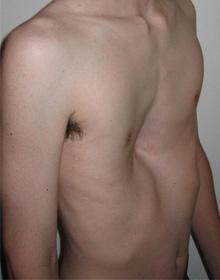 Pectus cavernatum can often be corrected non-surgically through a bracing procedure that applies pressure to the chest, gradually molding it into the correct position. But surgery to correct PE is a serious undertaking, and until recently, PE was not viewed as medically troubling enough to warrant a major operation. Pediatricians rarely advocated surgical correction, even in cases of severe deformity. As a result, patients suffered greatly, both with their feelings of shame and embarrassment, as well as physical effects that often went unrecognized, and which sometimes worsened over time. PE can compromise lung capacity and cause symptoms such as fatigue, shortness of breath, chest pain, and a fast heartbeat or chest murmur. While patients may not notice symptoms at rest, many experience symptoms upon exertion, leading them to withdraw from physical activities.
Pectus cavernatum can often be corrected non-surgically through a bracing procedure that applies pressure to the chest, gradually molding it into the correct position. But surgery to correct PE is a serious undertaking, and until recently, PE was not viewed as medically troubling enough to warrant a major operation. Pediatricians rarely advocated surgical correction, even in cases of severe deformity. As a result, patients suffered greatly, both with their feelings of shame and embarrassment, as well as physical effects that often went unrecognized, and which sometimes worsened over time. PE can compromise lung capacity and cause symptoms such as fatigue, shortness of breath, chest pain, and a fast heartbeat or chest murmur. While patients may not notice symptoms at rest, many experience symptoms upon exertion, leading them to withdraw from physical activities.
For years, the standard surgical correction of PE was the Ravitch procedure, in which an incision is made in front of the chest, the deformed cartilages are removed, and the sternum divided and elevated into the correct location. Typically a bar or strut is placed behind the sternum to maintain its position while the ribs and sternum heal. A change in thinking began about 20 years ago when Dr. Donald Nuss, a pediatric surgeon in Virginia, developed a minimally invasive procedure to correct PE. His approach accessed the chest wall through much smaller, less visible incisions in the patient’s side. From there, surgeons would insert one (or possibly two) surgical bars and stabilize them to reshape the sternum. After two to four years, when the chest wall had been fully reshaped and healed, they would remove the bars in another procedure.
While the Nuss procedure involves a painful post-operative period, it is a far less extensive procedure overall than the traditional open surgery, according to Lyall A. Gorenstein, MD, Director of Minimally Invasive Thoracic Surgery at NewYork-Presbyterian/Columbia University Medical Center. As increasing numbers of surgeons offered this procedure, more patients began undergoing corrective surgery that would transform their lives.
Among those early adopters was Charles J. H. Stolar, MD, Surgeon Emeritus and former Chief of Pediatric Surgery at Morgan Stanley Children’s Hospital of NewYork-Presbyterian (MSCHONY), who trained Dr. Gorenstein and other surgeons at NYP/Columbia in the Nuss procedure.
Surgery for PE is best performed when children are between age 12 and 18. Many adults who were not offered treatment as teenagers are now seeking correction, often because of its impact on exercise tolerance. Outcomes are excellent. In addition to the clear cosmetic benefit, many patients demonstrate improved heart and lung function after recovery. Patients can return to normal activity four to six months after surgery.
Not just for kids
Today NYP/Columbia’s pectus program, one of the largest and most experienced in the country, treats both adults and children with chest wall anomalies. Lawrence Bodenstein, MD, PhD, a pediatric surgeon at MSCHONY, and his colleagues treat children and adolescents, while Dr. Gorenstein treats older teenagers and adults. Fueling the program’s growth is widespread recognition by both doctors and patients that a) physical and psychological effects associated with chest wall anomalies are significant, and b) the benefits of treatment outweigh the costs and trauma associated with surgery.
For patients who require an open procedure, Dr. Gorenstein has modified the Ravitch procedure so it too is less invasive. Previously, the supports used to keep the sternum in place needed to be removed after several years. The bars currently used are secured to the chest wall in such a fashion that they can remain permanently in place, thereby avoiding the need for a second operation.
“In older patients and some young patients with complex chest wall deformities, the modified Ravitch we perform may be a better alternative to the Nuss repair,” says Dr. Gorenstein. “Because we have experience with both procedures, we can select the appropriate technique, based on the patient’s chest wall abnormality.”
“Chest wall anomalies can have profound physical and psychological effects,” explains Dr. Bodenstein. “It is hard to overstate the devastating psychosocial impact that PE and PC have. Chest wall anomalies tend to become more pronounced during adolescence, just as teens are becoming most concerned about their appearance. They try to hide their condition with bulky clothing, but gym class or going to the beach or pool can be a miserable experience.”
No longer viewed as simply a cosmetic procedure, surgery to correct PE is considered reconstruction of the chest to its normal form. “Along with the physiological gain,” Dr. Bodenstein explains, “correction of pectus abnormalities is incredibly rewarding. After teenagers have surgery, it is as if a light goes on — they are different people, their whole world brightens.”
