Guide to Parathyroid Surgery (Parathyroidectomy)
On Page Nav:
Reviewed by the physicians of Columbia’s Parathyroid Surgery Team, February, 2026
Parathyroid surgery, also called a parathyroidectomy, is a procedure to remove one or more of the parathyroid glands located in the neck. These tiny glands regulate calcium levels in the blood. When one or more become overactive — a condition called primary hyperparathyroidism — surgery is often the most effective treatment.
Key Info
- The parathyroid glands control calcium balance in the body.
- Primary hyperparathyroidism is commonly caused by a benign tumor (adenoma) on one or more of the parathyroid glands.
- Surgery is the only definitive cure for hyperparathyroidism.
What Are the Parathyroid Glands?
The parathyroid glands are four pea-sized glands located behind the thyroid in the neck. They produce parathyroid hormone (PTH), which helps regulate calcium levels in the blood and bones.
When one gland produces too much PTH, calcium levels in the blood rise. This increase can lead to symptoms such as kidney stones, bone loss (osteoporosis), abdominal pain, depression, or fatigue. Long-term untreated hyperparathyroidism increases the risk of fractures, kidney damage, and cardiovascular problems.
What is a Parathyroidectomy?
A parathyroidectomy is a surgical procedure to remove the overactive parathyroid gland(s). Depending on the case, surgery may remove:
- One gland (most common)
- More than one gland if multiple are overactive
- Rarely, all four glands, with part of a gland transplanted elsewhere in the body to maintain some function
Surgery is the treatment of choice because there are no medications or lifestyle changes that can reliably cure hyperparathyroidism.
How is Parathyroid Surgery Performed?
There are two main approaches:
- Focused parathyroidectomy: The surgeon identifies the location of the diseased parathyroid gland(s) before the operation and removes the diseased gland(s) during the surgery.
- Bilateral neck exploration: The surgeon explores both sides of the neck to examine all four parathyroid glands. The surgeon decides which gland(s) to remove based on their size, color, and texture.
Minimally Invasive Parathyroid Surgery
The typical incision made for parathyroid surgery is known as a "collar incision" in which a large incision (around 5 to 6 inches) is made stretching from one side of the neck to the other just above the collarbone. Minimally invasive parathyroid surgery refers to certain types of surgery in which the parathyroid is removed through very small incisions (around 1 to 1½ inches) using special techniques.
Intraoperative PTH Monitoring
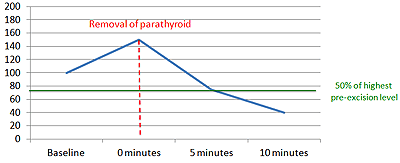
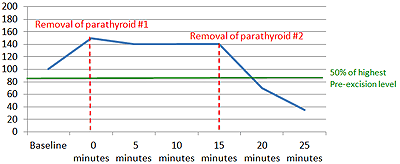
Parathyroid hormone (PTH) levels in the blood change very quickly because the hormone can be cleared from the blood within minutes. Surgeons use this fact to confirm that all diseased parathyroid tissue has been removed by measuring the PTH levels at certain times during an operation in a process called intraoperative PTH monitoring.
In the most common form of intraoperative PTH monitoring, the surgeon measures the PTH level:
- before starting the operation (i.e. baseline)
- before tying off the blood supply to the diseased parathyroid gland (i.e. pre-excision or time zero)
- 5 and 10 minutes after removing the diseased parathyroid gland.
Ten minutes after removing the diseased parathyroid gland, the PTH levels should drop by 50% or more from the baseline or pre-excision PTH level (whichever of the two is higher).
If the levels fall by more than 50%, then there is an approximately 98% chance that the patient is cured. If the levels do not fall by more than 50%, then there may be other diseased parathyroid glands and the surgeon will usually look again at the other 3 glands through the same small incision and make a decision about which one(s) to remove based on how abnormal they look.
What is Autotransplantation?
Having the equivalent of at least one normal-sized or functioning parathyroid gland is critical to maintaining the calcium levels in the body. Autotransplantation removes parathyroid tissue from its normal location and then places it into the muscles of the neck or forearm. The autotransplanted parathyroid gland then lives and functions in the new location.
Autotransplantation is performed if:
- The removed parathyroid gland is the patient's last parathyroid (i.e., the patient has had a previous operation in which three parathyroid glands were removed),
- The patient has four hyperactive parathyroid glands that need to be removed
- A normal parathyroid gland is removed during surgical removal of the thyroid gland
If the autotransplanted parathyroid is a normal parathyroid gland, it is often put in one of the neck muscles. If the autotransplanted parathyroid is a hyperactive parathyroid gland, it is often put in the forearm muscle because if the hyperactive autotransplant grows or becomes too active again, it is easier and safer to remove it from the forearm than the neck.
The autotransplanted parathyroid gland takes about 4 to 6 weeks to start working again; during this time, patients will need to take calcium supplements (typically pills, but sometimes intravenous or IV) and calcitriol (vitamin D).
Cryopreservation of Parathyroid Tissue
In certain cases, the surgeon can freeze and save some of the parathyroid tissue that is removed in a process called cryopreservation. This frozen parathyroid tissue is then stored in the freezer under sterile conditions as an insurance policy. If the patient ever needs more parathyroid tissue in the future, the surgeon can thaw it out and autotransplant it back into the body, usually in the forearm.
How Do I Prepare for Parathyroid Surgery?
In addition to the localizing tests that are designed to identify the diseased parathyroid gland(s), prior to the operation, patients will need certain pre-operative testing to make sure that they are healthy enough and properly prepared for an operation. The typical recommendations for pre-operative testing include:
- Blood tests done within 30 days of the operation
- CBC (complete blood count)
- BMP (basic metabolic profile)
- B-HCG (blood pregnancy test) for menstruating females
- Coagulation profile if the patient is on blood thinners or has a bleeding disorder
- EKG done within 3 months of the operation for patients older than 40
In addition, patients may require additional tests in certain situations to help plan the operation. It is not common to need these additional tests, but they may include:
- Fiberoptic laryngoscopy: This test allows the surgeon to look at how well the vocal cords are moving by passing a thin flexible camera through the nose into the airway. This test is used in patients with hoarseness, a previous neck operation, or cases of advanced cancer.
Patients with other significant medical issues may be asked to visit with their medical team to obtain a letter of medical clearance. The medical clearance allows the patient's medical team the opportunity to optimize the patient's health prior to an operation and allow the specialists to make recommendations for how best to care for the patient's other medical issues during the peri-operative period.
What Type of Anesthesia is Used?
Parathyroid surgery is usually performed under general anesthesia. Some centers also offer local anesthesia with sedation for selected minimally invasive cases.
How Long Does Parathyroid Surgery Take?
- A minimally invasive surgery typically takes 30 minutes to 1 hour.
- An open exploration may take 1 to 2 hours.
Most patients go home the same day.
What are the Risks?
As with any surgery, parathyroidectomy carries some risks, though complications are uncommon when performed by experienced surgeons. Risks may include:
Bleeding in the neck
As with any operation, there is always a chance of bleeding. The average blood loss for this operation is less than a tablespoon and the chance of needing a blood transfusion is extremely rare. In the hands of experienced surgeons, the risk of bleeding is less than 1%. However, bleeding in the neck is potentially life threatening because as the blood pools, it can push on the windpipe or trachea causing difficulty breathing.
Due to this rare risk of bleeding, patients should be observed for at least 4 hours by highly trained recovery room staff. If there is no sign of bleeding and the patient feels well, he or she may go home. Once at home, patients and their friends/family should watch for signs such as difficulty breathing, a high squeaky voice, swelling in the neck that continues to get bigger, and a feeling that something bad is happening. If any of these symptoms happen, the patient should call 911 first and then their surgeon.
There will often be a little swelling around the incision site for a few weeks after the operation. A small amount of swelling is part of the normal healing process. The natural reaction to surgery is to form scar tissue that will become firmer in the first few weeks and then will slowly soften up. This swelling is typically only 1 to 2 finger breadths in size and should not get significantly bigger. If the swelling continues to get bigger, especially if it is growing quickly over a couple of hours, contact your surgeon immediately.
Over the next few months, the swelling and scar tissue will disappear and the area should look and feel just like the normal skin.
Hoarseness (Recurrent laryngeal nerve injury)
There are two nerves called the recurrent laryngeal nerves that run just behind the parathyroid. These nerves control the vocal cords. If one of these nerves is injured, the voice may become hoarse.
Temporary hoarseness usually gets better within a few weeks, but can take up to 6 months to resolve.
Hypocalcemia (Hypoparathyroidism)
After parathyroid surgery, there is a small chance that the blood calcium levels can become lower than normal, a situation called hypocalcemia. This typically only happens if a person has 4 hyperactive glands and the patient has 3 to 3.5 of the glands removed. In some cases, the diseased parathyroid gland(s) that is removed has suppressed or temporarily shut down the other parathyroid glands.
Hypocalcemia can cause symptoms such as numbness and tingling (especially around the lips and in the hands and feet) as well as cramping and even "locking" of the hands and feet. It is important to note that numbness and tingling may be caused by something other than a parathyroid problem. If a patient has symptoms caused by low blood calcium, the surgeon may prescribe extra calcium and a vitamin D supplements.
Other risks of parathyroid surgery include wound infections and seromas, which are collections of fluid under the incision. Wound infections happen in about 1 out of 2000 operations (far less than 1%) and because of this low risk, the routine use of antibiotics is not needed. Seromas happen rarely and usually disappear within a few weeks. If the seroma is large, the surgeon may drain it with a small needle.
The risk of having any of these complications depends on the experience of the surgeon. Although the risk of these complications cannot be eliminated entirely, they can be minimized in the hands of an experienced parathyroid surgeon.
Is Parathyroid Surgery Painful?
Most patients will feel like they have a sore throat for the first few days after the operation, especially when swallowing. Some people experience a dull ache, while others feel a sharp pain.
The Parathyroid Center recommends taking Tylenol, Motrin, or Advil as the bottle directs around the clock for the first few days (as long as the patient's overall health allows it).
The vast majority of patients do not require narcotic pain medications.
What is Recovery Like?
- Most patients can return to normal activities within a few days.
- Temporary sore throat or mild neck discomfort is common.
- Patients should be able to eat their normal diet, but most prefer softer foods for the first few days.
- Calcium levels are closely monitored after surgery. Some patients may need temporary calcium or vitamin D supplements.
- Symptoms of high calcium, such as fatigue or bone pain, usually improve quickly once
How Long Does Recovery Last?
Many patients start eating, drinking, walking around, and doing their normal activities the night of the operation. However, patients must avoid heavy lifting, swimming, or soaking in a bathtub for 1 week after the operation. For minimally invasive parathyroid surgery, the incisions should heal completely within 1-2 weeks.
Patients should call their surgeon's office to make a follow-up appointment approximately 2 to 3 weeks after surgery. It's important to monitor blood calcium levels after surgery to ensure a return to normal levels.
Will There Be Scarring?
Minimally invasive parathyroid surgery uses very small incisions (around 1 to 1½ inches), minimizing the amount of scarring. Skilled surgeons can "hide" the incision in a natural skin crease, which acts like camouflage. Most people will not be able to notice the incision once the redness fades away.
There will often be a little swelling around the incision site for a few weeks after the operation. A small amount of swelling is part of the normal healing process. The natural reaction to surgery is to form scar tissue that will become firmer in the first few weeks and slowly soften. This swelling is typically minor; if it continues to get bigger, especially if it grows quickly over a couple of hours, contact your surgeon immediately.
Over the next few months, the swelling and scar tissue will disappear, and the area should look and feel like normal skin.
Scar Gallery
The Scar Gallery below shows examples of minimally invasive parathyroid surgery from Columbia patients.






What is the Outlook?
Parathyroid surgery has a very high cure rate — over 95% when performed by an experienced surgeon. Successful surgery can:
- Normalize calcium levels
- Improve bone density
- Reduce kidney stone risk
Next Steps
If you or a loved one has been diagnosed with a parathyroid condition, the team at the Columbia Parathyroid Center can help.
Columbia Parathyroid Center surgeons perform minimally invasive parathyroid surgery in over 97% of patients, and 95% of our patients go home same-day after a 4-hour observation period in the recovery room. Our surgeons have more experience, which means better results and fewer complications.
To learn more or schedule an appointment with Columbia's Parathyroid Surgery team, call 212-305-0444 or request an appointment online. We accept a number of insurance plans, and our team can help confirm your coverage.
Related
- The Parathyroid Glands: What are they?
- Primary Hyperparathyroidism
- Secondary Hyperparathyroidism
- Parathyroid Cancer
- Re-operative Parathyroid Surgery
This content has been created by Columbia’s Health Guide Team. Learn more about our efforts to bring you the clearest, most accurate, and most human health resources available.
