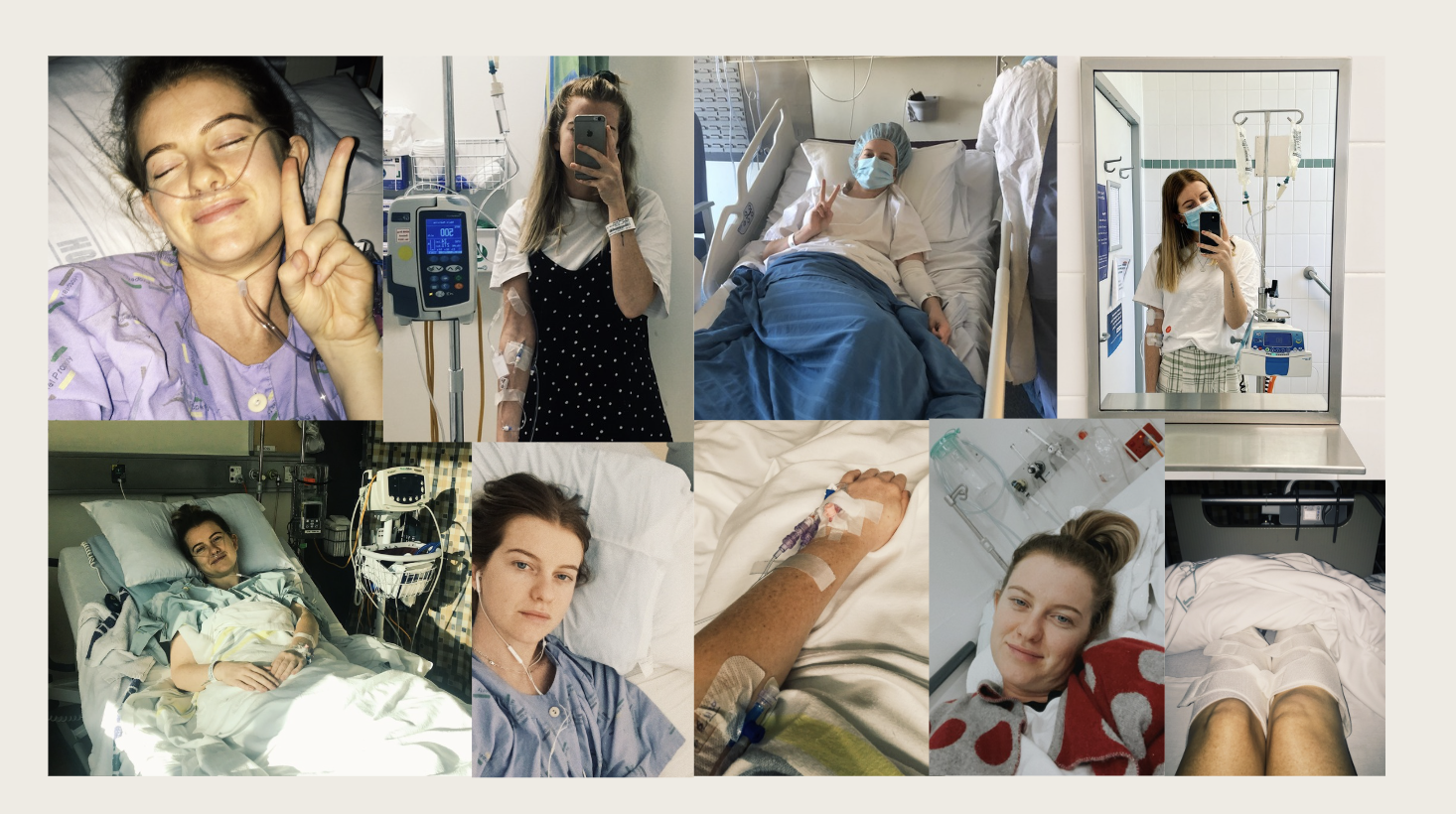
On a recent afternoon, not long after she crossed into her second trimester, filmmaker Rachel Ross found herself doing something she hadn’t been able to do in years: walking through New York without planning every exit.
There was no subtle calculation of where the nearest bathroom might be. No inventory of symptoms. No low, constant negotiation with her own body. She moved the way people do when they are not thinking about it at all—up the subway stairs, onto the street, back into the rhythm of the city. But for a long time, that kind of movement had felt far out of reach.
“I haven’t been in the ER. I haven’t had any crises,” she said. “For me, that is massive.”
Rachel grew up in New Zealand, in a family and familiar culture where pain—especially the kind that comes with being a young woman—was something you learned to absorb. “You don’t want to be dramatic,” she said.
What You Learn to Ignore
For years, she had two parallel experiences unfolding in her body. There were the gynecologic symptoms, like severe, destabilizing periods that left her vomiting, fainting, and unable to stand. And then there were the gastrointestinal ones: bleeding, urgency, a creeping sense that something was not right.
Neither was investigated with much urgency. The bleeding was attributed to hemorrhoids, and per usual, the pain was something she was expected to tolerate. She learned, as many women do, to translate what she felt into something more acceptable.
“I began to doubt my own body,” she said.
By the time she arrived in the United States in 2017, what had been manageable—or at least survivable—was beginning to break open. The symptoms escalated quickly, bleeding worsened. She started losing control of her bowel in ways that were both physically and socially disorienting, sometimes humiliating.
In New York, she found herself moving through the city with a kind of vigilance that is hard to describe unless you’ve lived here, a massive city with virtually no public restrooms. Calculating distances, scanning for bathrooms, improvising when there were none. Once, in a store, she sat down on the floor to keep herself from having an accident.
“It’s such an inaccessible city when you need something immediately,” she said. Still, even then, she didn’t have a name for what was happening in her body.
When Illness (Finally) Becomes Impossible to Miss
Later, after a trip to Los Angeles, things tipped into something much more severe. She was admitted to the hospital, her blood work suggesting infection and symptoms mimicking something potentially life-threatening. It took days and a cascade of testing before she was diagnosed with ulcerative colitis—already in an absolutely severe, pan-colonic form.
“They told me if I had gotten on that plane back to New Zealand, I might not have made it,” she said.
And immediately, her life reorganized around the disease. Hospitalizations, medications, side effects that felt as destabilizing as the illness itself. At one point, the drugs she was prescribed (intended to suppress an overactive immune system) left her with symptoms she described as “chemo-like”—hair loss, vomiting, insomnia, migraines.
It wasn’t until much later, when options were running out, that she started on infliximab (Zymfentra), a biologic that she understood as her last chance to avoid surgery. It worked. The bleeding eased and volatility settled. For the first time, she wasn’t losing her hair or vomiting throughout the day.
Rachel doesn’t hedge when she talks about it. She calls it the drug that saved her colon, her "miracle drug," even now. "That's what I have called that medication for 8 years," she explained. It brought her close to remission, but not all the way.
She stabilized, eventually, but “I never reached remission."
Even when things were considered mild clinically and scopes showed only low-grade inflammation, her symptoms never ceased. Rachel’s stool tests, measuring markers like calprotectin, were at times off the charts.
A Chance Encounter and a Clinical Trial
Years later, Rachel found herself in New York again. She and her husband were in the city temporarily, trying to decide whether they could make a life here, when a last-minute housing situation led them to an apartment swap.
In a twist that might be considered too narratively neat for fiction, the man whose apartment it was had just undergone a procedure: the implantation of a sacral nerve stimulator as part of an early clinical trial. He told her about it casually, in passing.
“I’d never met anyone with ulcerative colitis before,” she said. “And suddenly here was someone who had just done this thing.”
The device itself isn’t new. Sacral nerve stimulation has been used for years to treat conditions like fecal incontinence. It’s a small implant, placed under the skin, that delivers daily electrical pulses to the sacral nerve. But the application is entirely new.
At the Inflammatory Bowel Disease Center at Columbia, colorectal surgeon Marco Zoccali, MD, is leading the BOOM-IBD2 clinical trial to explore whether stimulating that nerve, which is part of the broader parasympathetic network that helps regulate the gut, could do more than manage symptoms. The hope is that it might actually modulate inflammation itself by rebalancing it entirely.
“It’s like a pacemaker for the gut,” said Dr. Zoccali.
For Rachel, the appeal was immediate and complicated. She had spent years managing her disease with medication, never quite reaching stability, often trading one set of symptoms for another. The idea of something that worked through the body’s own signaling pathways felt, at the very least, worth considering.
It also required a leap around the world. Within weeks, she and her husband had decided to move. They sold what they could back in Australia, packed the rest into storage, and returned to New York under a compressed timeline dictated by the trial’s enrollment window. She arrived, signed the necessary paperwork, and went into surgery the next day.
“I remember laughing as they were putting me to sleep,” she said. “I felt very at ease.”
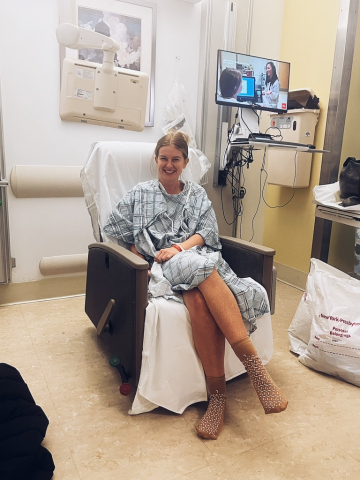
For the First Time
The recovery was slower than she expected. For the first several weeks, her movements were restricted. She couldn’t bend or lift, couldn’t risk dislodging the device as it settled into place. Her world contracted down to a small apartment, the sounds of the city filtering in from outside.
Maybe it’s the filmmaker’s way, but there was something almost cinematic about it—New York still just beyond reach, her body recalibrating in ways she couldn’t yet feel.
The change, when it came, was gradual. Her symptoms softened first. Then her lab values began to shift. The markers that had once been erratic started to stabilize. Over time, the data and her experience began to align in a way they hadn’t before.
And then, at the end of the trial, she had a full colonoscopy, and they saw nothing. No active inflammation. Only the scar tissue of what had been there before. “I’d never had that,” she said. “Ever.”
The Healing Power of Story
Around the same time, Rachel began writing a film.
It’s called Good Girl Greta, and it follows a young woman in New York who, in the middle of an ordinary day, loses control of her body in a way that forces everything into the open. The film moves through playgrounds, emergency rooms, and crowded streets, tracking both the external chaos of the city and the less visible unraveling happening inside her.
It is, in most ways, a reworking of Rachel’s own experience. “Women are taught this early,” she said. “Be accommodating. Be capable. Be quiet.”
In the film, as in her life, the question becomes harder to avoid: When do you decide to trust your own body over everything you’ve been taught to ignore?
Rachel is over six months pregnant now. It happened more easily than she expected, given her history of ulcerative colitis, endometriosis, and years of instability. She is, as far as she knows, the first patient in the trial cohort to become pregnant after receiving the implant.
“We got pregnant really quickly,” she said. “I’m just so, so grateful.”

There is still uncertainty. There always is. But the device remains in place, and it’s working. While the trial is set to enter stage 2, research is ongoing. The outcomes, across patients, are still being understood. But for now, her life feels different, steadier, and Rachel is full of gratitude.
The film is moving forward, too. Set to begin production this summer, on a timeline shaped as much by her pregnancy as by anything else. It’s being built the way many first films must be—piece by piece, through community, urgency, and creating art built from the depths of one’s own experience.
“I spent years being told I was fine,” she said. “So I believed that I was.”
Now, she moves through the city without that same negotiation because something has shifted in how she listens to herself. The body, it turns out, had been speaking clearly all along.
More About the BOOM-IBD2 Trial
The BOOM-IBD2 trial is a prospective, single-arm, multicenter pivotal trial to evaluate the effectiveness of sacral nerve stimulation (SNS) in patients with ulcerative colitis. The trial is currently open to enrollment. The SNS device used in this trial is limited by Federal (or United States) law to investigational use. Click here for more information about the BOOM-IBD2 Trial.
Study Contact:
Call (212) 342-4102
Claudia Musat, MD: cm2065@cumc.columbia.edu
Related:
- How a New Clinical Trial for IBD Is Changing Frank’s Life
- Dr. Marco Zoccali Explains Groundbreaking Clinical Trial for IBD
- Dr. AI: What Is the Best Way to Treat Hemorrhoids?