Robotic living donor liver surgery doesn’t begin at the hospital, nor with the robot or even the surgeon. It begins, as transplant surgery always does, with a person who wants to give. Someone who has decided that they might be able to help and chooses to take the step. That decision sets everything else in motion.
At Columbia, the momentum has now reached something no other program in the country has: one hundred robotic living donor liver transplants. The fastest-growing program is the first to get there. But, in so many ways, the team is still just getting started.
“This is a great achievement for the entire Living Donor Liver team,” says Jason Hawksworth, MD, Surgical Director of Adult Liver Transplantation and Chief of Hepatobiliary Surgery. “It’s also a testament to our donors and their willingness to put themselves at risk to save someone else’s life.”
“It’s really just inspiring,” says Alyson Fox, MD, Medical Director of Adult Liver Transplantation, who has spent the last fifteen years with the living donor program. “And it makes me really proud to work here.”
Changing the Future of Living Liver Donation: A Conversation about Columbia’s All-Robotic Approach
Lowering the Barrier
For decades, living liver donation asked something enormous of donors—a major operation, a long recovery, and a visible scar. The evolution to robotics didn’t change the generosity required, but it did change the cost of that generosity.
“We saw early on—this is really better for patients,” Dr. Fox says.
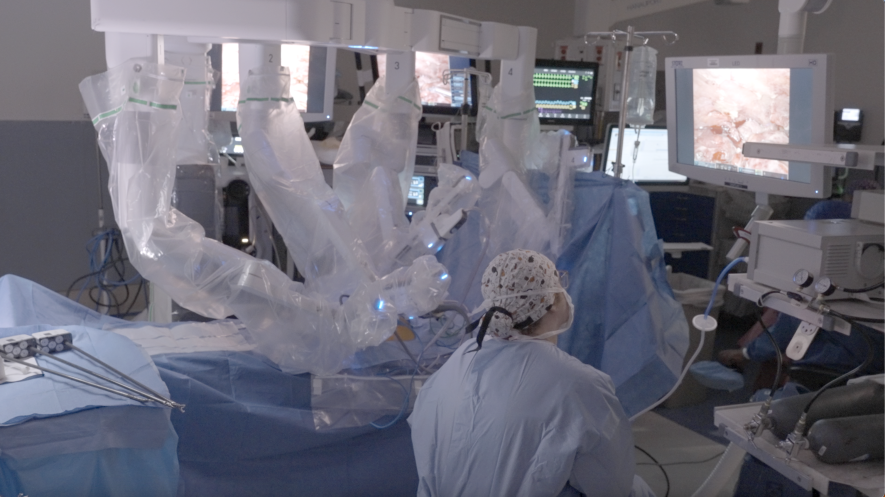
“The difference between a robotic and a traditional open liver surgery is really night and day,” explains Dr. Hawksworth.
Where donors once stayed in the hospital for a week or more, they now leave in a matter of days. Where surgery once required a large incision and rib spreading, it now happens through small ports, with the liver removed through a low, contained incision.
“It allows the donor to functionally return to normal life very quickly,” he continues. “And I think this makes the idea of donating much more appealing to people who are healthy and living their lives.”
The People Who Hold It Together
If liver transplant is, as Dr. Fox calls it, “the ultimate team sport,” then this program is built by the people who make it possible, everyone working behind the scenes.
“There’s an immense amount of planning,” Dr. Hawksworth says. Multiple multidisciplinary meetings, imaging, lab work, coordination between teams who follow different patients but are tied to the same outcome.
On the day itself, it’s not one surgeon. It’s two. Plus, specialized nurses, scrub techs, anesthesia teams, all trained for this specific operation. “No one person can do this on their own,” Dr. Fox says. While some of that work is visible, much of it isn’t.
There is the living donor specialist who becomes the bridge between questions and answers, between fear and clarity. “My role is to navigate the donor through the process,” says Jennica Kim, who guides patients from first inquiry through surgery and beyond.
There is the nurse coordinator, reading through histories and lab results, assembling a picture of someone’s life and health, then bringing it into a room full of experts to decide, collectively, whether to move forward. “I’m very protective of donors,” says Lesly Dumé, RN, BSN. “This is their ship, and we are their crew.”
There is the social worker, Sonia Scott, MSSW, LCSW, whose job is not only to move things along, but sometimes to stop them. “To make sure that all of the donors are well informed,” she says. “And ultimately back out if this is something that they feel they cannot move forward with.”
Protection is not a side note here, but the very foundation. Every donor must be healthy, and every donor must choose this for themselves. “The most important aspect of living donor liver surgery is safety. It has to be safe for that donor,” Dr. Hawksworth says. “We never compromise on donor safety—even for the outcome of the transplant.”
And that philosophy shows up from start to finish. “Our donors are our VIPs,” Dr. Fox says. It’s policy and practice—the anchor resting underneath every case. And every part is methodical, repetitive, and deliberate.
One Gift, Three Futures: Inside the 15-Hour Dance of the First Living-Donor Domino Split-Liver Transplant in Adults
Ask anyone on the team (even the surgeons) what stays with them, and the answers aren’t about the surgery itself. They’re all about moments, that human connection with recipients, donors, and their families, before and after the operation.
“Just hearing that they’re doing well and have moved on with their normal lives is everything,” Kim says.
Sometimes it’s a phone call, weeks later, where both donor and recipient are on the line, talking at once, both recovering. Others, a holiday card sent years down the road, now filled with photos of children who did not yet exist. That moment in clinic when someone realizes they are a match.
“There are tears; it’s very raw,” Dumé says. “I love seeing this process begin and then come to a place where they’ve literally saved someone’s life. The recipient, the donor, they’re changed forever. We’re changed, too.”
The journey builds bonds for life. “We feel like part of the family,” Dr. Fox says.

What One Hundred Means
On its face, the number is straightforward: one hundred robotic living liver operations. But that number is also one hundred times this entire system worked. Each one required coordination across surgeons, hepatologists, nurses, coordinators, social workers, and more.
It’s one hundred times a person chose to give something of themselves to save a life. One hundred times a team decided it was safe enough to proceed, and then one hundred successful operations.
“There’s nothing more satisfying,” Dr. Hawksworth says, “than completing a living donor operation and then seeing a successful transplant outcome on the other end.” That moment is the point of everything.
Even so, there is very little sense of arrival with this group—the focus is still on refinement. Conversations about moving toward even smaller incisions, better technology and tools, fewer complications. “I think that’s the future,” Dr. Fox says. “Making it safer for patients, refining it over and over again.”
“Our goal is zero complications in our donors,” Dr. Hawksworth says.
And beyond the technical work is something perhaps even more important: access. Fewer than seven percent of liver transplants in the U.S. currently come from living donors. The hope is to change that and move closer to what kidney transplant has already shown is possible.
“I’m hoping this will improve the number of people who are willing to donate,” he continues. “There’s such an important job in sharing all of this. So many people still don’t know this is an option at all.”
And that’s what living liver transplant ultimately depends on. People knowing this is possible, and people stepping forward. The 100th robotic surgery is a major milestone. But it is also proof that this—done carefully, repeatedly, and together—works.
Related:
- One Living Donation Saves Three Lives: NewYork-Presbyterian/Columbia Performs the First Domino Split-Liver Transplant in Adults in the U.S.
- Bots for Tots: The First Program in the U.S. for Robotic Liver Surgery in Children
- Caracas to Santo Domingo: Creating Access to Pediatric Liver Transplant from the Ground, Up

