As we bid farewell to another transformative year, pride and gratitude swell among us. We encourage everyone to take a moment to reflect on all the remarkable strides made in patient care, from the lab to the operating room, in 2023.
Here at Columbia, these past twelve months have been a testament to the dedication of our specialists, clinicians, nurses, administrators, support staff, and colleagues across borders who make it all happen. Thank you for all you do, and cheers to what is bound to be another inspiring year ahead.
The Smallest Cuts, The Biggest Impact
Saving Two Babies’ Lives With One Pioneering Approach to Heart Valve Transplantation
Meet Mia Skaats and Brooklyn Civil, two infants whose chance encounter in a playroom at NewYork-Presbyterian Morgan Stanley Children’s Hospital marked the beginning of an extraordinary journey. Born strangers but united by rare, life-threatening heart conditions, these resilient kids became the pioneers of the first-ever domino heart valve transplant in infants. Led by the expertise of a multidisciplinary team from pediatric cardiology and pediatric heart surgery, the groundbreaking procedure not only saved lives but also showcased the power of teamwork, timing, and mindful innovation. Don’t miss their story featured on the Today Show.
Total Artificial Heart Revolutionizes Heart Transplant Surgery
“The colleagues that you have here, the dedication that they show and how smart they are and how hardworking they are, is unbelievable. Without my colleagues, I might as well go do something else.”
— Dr. Emile Bacha
Dr. Emile Bacha, Chief of the Division of Cardiac, Thoracic, & Vascular Surgery, made history by performing the first-ever total artificial heart (TAH) implant on one of the youngest pediatric patients in the Northeast. This remarkable feat not only marks a significant step forward in pediatric cardiac interventions but also emphasizes the sheer dedication to developing life-saving solutions for the most complex cases.
Liver Team Creates Access to Pediatric Liver Transplant in the Dominican Republic from the Ground, Up
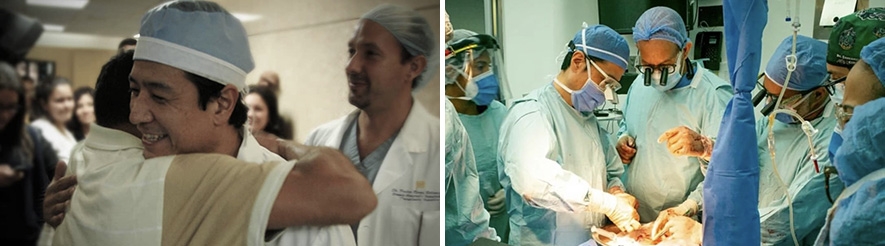
Dr. Tomoaki Kato, Chief of Abdominal Organ Transplant and Hepatobiliary Surgery, met transplant surgeon Dr. Pedro A. Rivas nearly two decades ago. Together they developed the first pediatric liver transplant program in Venezuela. Then they created the foundation FundaHigado with the mission to bring life-saving liver transplants to children in every country without access. They recruited Dr. Mercedes Martinez to tackle surgical development in the next country, the Dominican Republic. After six years of hard work on the ground, through a pandemic, they successfully transplanted the first children to ever receive liver transplants in the country this year at the newly developed program in Santo Domingo. The transplant was featured on Telemundo this fall.
Dr. Jenn Kuo Teaches Radiofrequency Ablation (RFA) Across the Continent
As the leader of Radiofrequency Ablation (RFA), a non-surgical procedure that can safely and effectively treat non-cancerous thyroid nodules, Dr. Jennifer Kuo traveled all over North America this year teaching the technique to physicians of varying specialty backgrounds. Her leadership in this field has made Columbia one of the designated training centers for interventional endocrinology in the country. She also served as the inaugural president of the North American Society of Interventional Thyroidologists (NASIT), a new society dedicated to the emerging field of interventional endocrinology. Furthering the mission is to promote excellence in thyroid care while advancing the latest in cutting-edge practice.
Fetal Surgery Innovations Are Providing Big Solutions to Tiny Patients
Dr. Vincent Pierre Duron, Co-Director of Fetal Therapy at Columbia and Surgical Director of the Pediatric ICU, is a leader in the field of fetal surgery, particularly in treating conditions like spina bifida and congenital diaphragmatic hernia (CDH). His work has furthered the development of fetoscopic repair, a surgical method that uses miniaturized instruments, scope, and camera to repair fetal abnormalities through the uterus before birth. The procedures are optimizing outcomes for both the fetus and the mother, improving survival rates, and preventing complications associated with severe CDH.
Pioneering Approach of Kidney Autotransplantation for Complex Kidney Disorders Offers Big Hope
For some rare kidney disorders, traditional surgical approaches may risk significant kidney damage due to tumor location or size. This year, Dr. Lloyd E. Ratner established the first and only autotransplantation program in the New York Metro area. Where surgeons remove the diseased kidney minimally-invasively, repair it outside the body, and transplant it back in. It’s a revolutionary approach that brings together experts from vascular surgery and urology and provides hope for those who might otherwise face kidney loss or prolonged suffering.
Year of the Robot
Complex Liver Surgery Has Gone Robotic, and the Benefits Are Vast
A trailblazer in the field of robotic liver surgery, Dr. Jason Hawksworth’s expertise is transforming the landscape of hepatobiliary surgery. As the new Surgical Director of Adult Liver Transplantation and Chief of Hepatobiliary Surgery at Columbia, Dr. Hawksworth is among the select few surgeons in the U.S. who perform intricate liver surgeries entirely with robotic technology. His role at Columbia marks a new era, offering patients access to cutting-edge robotic liver surgery, and advancing the standards of patient care.
Robotic Repair for Mitral Valve Disease Upends What's Possible
The architect behind the robotic mitral valve repair program at Yale, Dr. Arnar Geirsson joined us as the leader of the Robotic Cardiac Surgery Program earlier this year. His work is reshaping the landscape of mitral valve surgery, taking minimally invasive techniques, and evolving to offer even safer and more effective alternatives to traditional mitral valve repairs.
The First Robotic Kidney Transplant Is a Testament to Lifelong Friendship

This summer, another robotic surgery milestone was achieved. John Kennedy received the first robotic kidney transplant at Columbia. Robot-assisted surgery is an incredible advancement in the field of transplant. It allows us to provide even more options to patients and improve recovery time. But most importantly, through the love of Declan, his brother-in-law, John was given back his life.
Lab Takes The Lead
Groundbreaking Study for Treating IBD Prepares to Enter Phase III
"This could be a tool that would cure the disease, not just manage the symptoms."
— Dr. Marco B. Zoccali
The IBD Center is pioneering a groundbreaking approach in the treatment of Crohn’s Disease and ulcerative colitis through a nationwide study on sacral nerve stimulation (SNS). While SNS has been a conventional therapy for fecal incontinence, Columbia is the first to utilize it for inflammatory bowel disease (IBD) in the BOOM-IBD trial. Dr. Marco B. Zoccali, the principal investigator, explains that SNS, stimulating the sacral nerve, modulates impulses of the parasympathetic system, potentially toning down inflammation. Initial trials showcased remarkable results for this non-pharmacological alternative. With the hope of achieving remission, this study introduces the possibility of a cure rather than symptom management for IBD.
A Clinical Trial Breakthrough Shows There Is No Advantage to Mastectomy for Many Breast Cancers
In a paradigm-shifting breakthrough, the I-SPY trials, a groundbreaking neoadjuvant treatment approach for locally advanced breast cancer, spurred an unexpected discovery: there may be no benefit to mastectomy over lumpectomy in these cancers. Dr. Roshni Rao, Chief of Breast Surgery, regards these findings as a transformative leap toward personalized, more nuanced, and potentially surgery-sparing approaches to breast cancer treatment.
Researchers Find Link Between Serotonin and Heart Valve Disease
A crucial link has been revealed between serotonin and degenerative mitral regurgitation (DMR), a common heart valve disease. The multicenter study, co-led by Columbia’s Giovanni Ferrari, PhD, and CHOP’s Robert J. Levy, MD, explores the role of serotonin in accelerating DMR. By analyzing clinical data and mitral valve biopsies, they discovered that the use of selective serotonin reuptake inhibitors (SSRIs) was associated with severe mitral regurgitation requiring surgery at a younger age. Genetic analysis identified a specific variant linked to increased sensitivity to serotonin, emphasizing the potential for genotyping to assess patients for low serotonin activity and the need for early mitral valve surgery. Paving the way for personalized treatment approaches and enhanced preventive measures.
Vaccine for Pancreatic Cancer Enters Phase II of Clinical Trial
“I'm a hopeless optimist, so I do find it very exciting. And the very preliminary results from the Phase I trial were striking enough to make the New York Times. It feels great offering it to people because it's hard to think of a significant downside. And there's the potential for real upside.”
— Dr. John Chabot
A groundbreaking Phase II clinical trial for a mRNA neoantigen vaccine for pancreatic cancer is underway. With a mortality rate of nearly 90 percent, this could be a transformative development in the treatment of pancreatic ductal adenocarcinoma (PDAC). Building on Phase I success, where a custom-made vaccine induced a measurable immune response in half of operable pancreatic cancer patients, Phase II expands to include many institutions across the country. This November, Dr. John A Chabot, Chief of GI/Endocrine Surgery, enrolled our first participant.
Expanding Access to Personalized Care Bridges Experts Across Specialties
A New Multidisciplinary Liver Tumor Clinic Advances Individualized Care
We launched a multidisciplinary Liver Tumor Clinic at Columbia this year. The Liver Tumor Program brings together a team of specialists from Columbia Surgery and Herbert Irving Comprehensive Cancer Center (HICCC), which includes hepatobiliary surgery, medical oncology, radiation oncology, interventional radiology, and hepatology. As one of the most specialized liver tumor clinics in the nation, this group of experts collaborates to establish personalized treatment and serves as a singular destination for the comprehensive treatment of liver tumors.
NYP launched a new podcast this year. An episode with Dr. Alyson Fox: Surprising Facts About Organ Donation
Lung Cancer Screening Center Aims to Target Lung Cancer Before Symptoms, When Still Treatable
“I can't emphasize this enough, patients will live longer if they're actively screened in the Lung Cancer Screening Program, not just for lung cancer, but for overall survival.”
— Dr Payne Stanifer
The criteria for lung cancer screening have expanded to include more people at risk who show no symptoms or active signs of lung cancer. It’s a huge improvement to pre-cancerous care, and why Dr. Payne Stanifer has developed a new Lung Cancer Screening Program with offices expanding to Bronxville and Hudson Valley locations. The original lung cancer screening trial showed a 20 percent lung cancer survival advantage for those who participated in routine screenings, and a nearly 10 percent overall advantage due to unexpected findings unrelated to lung cancer. Screening saves lives.
American Academy of Pediatrics Has Caught Up to the Latest in Treatment for Childhood Obesity
Earlier this year, the American Academy of Pediatrics updated their treatment guidelines for pediatricians and general practitioners to officially include earlier recommendations for weight loss surgery in children with obesity. Dr. Jeffery Zitsman, Director of the Center for Adolescent Bariatric Surgery, advocated for this change and highlighted the importance of surgical treatment of severe obesity in children and adolescents.
Spanish-Speaking Outreach Grows at the Center for Metabolic and Weight Loss Surgery
Bariatric surgeon Dr. Francisco Guzman-Pruneda was recognized as a 2023 Castle Connolly Top Hispanic and Latino Doctor. He shared his perspective on how being a Latino physician adds to his ability to serve patients, “What’s quite unique about New York City is the fact that over a quarter of its population is Spanish-speaking. To me, being able to provide direct care to my patients helps me build a stronger relationship with them,” said Dr. Guzman. “I feel this brings better outcomes, more satisfaction, and better understanding for patients and their families.”
Oncoplastic Surgery Creates a Personalized Approach to Breast Conservation
“When I see new breast cancer patients, I try to give a 360° approach. It’s important for me to assess not just the disease, but the person and what their goals are, before going forward.”
— Dr. Lisa Weichmann
With a better understanding of breast cancer’s genetic and molecular basis, the fields of oncologic breast surgery and plastic surgery are collaborating to provide patients with oncoplastic care that focuses as much on the quality of life as the efficacy of treatment. It’s a totally new approach that packs immense benefits.
The Ozempic Effect Brings New Specialized Weight Loss Clinic
Treatment for obesity is changing. Ozempic is a drug used to treat diabetes; now, millions of people are using it to lose weight. The Center for Bariatric and Weight Loss Surgery opened a clinic dedicated to obesity treatment with medications like Ozempic, Mounjaro, and Wegovy. Chief of Minimal Access/Bariatric Surgery, Dr. Marc Bessler, gave a comprehensive interview about how these drugs work, the differences between medical and surgical treatment for obesity, risks, benefits, and all the questions in between.
A Vascular Expert Responds to NYTimes Article on Predatory PAD Treatments
This summer, the New York Times exposed a predatory network of medical device companies bankrolling private clinics and paying doctors to perform procedures on patients with peripheral arterial disease (PAD). Many patients received procedures they did not need for a condition that doesn’t often require surgical intervention. Vascular surgeon, Dr. Nicholas Morrissey, was one of the first experts to respond with a comprehensive overview of PAD treatment and advice for patients seeking vascular care. The interview was widely shared and well-received.
New Surgical Oncology Forum Develops Greater Holistic Understanding of Disease for Clinicians
Surgical oncology is an area of expertise that expands on the surgical treatment of various cancers with a deep understanding of the disease itself, not just how to surgically fix it. Dr. Sam Yoon, Chief of Surgical Oncology, started a Surgical Oncology Forum this year to expand understanding of cancers in all parts of the body, from gastric cancer and sarcoma to the thyroid and lungs. These free, one-hour webinars feature experts on the cutting edge of their fields and are available on-demand to clinicians, researchers, and healthcare professionals who care for patients with cancer worldwide.
Reflection Makes Way for Celebration
Dr. Craig Smith Took Pen to Paper with New Memoir
Dr. Craig R. Smith, Chair of the Department of Surgery, released a book this year. Among the many insights, what we come to learn in Nobility in Small Things: A Surgeon’s Path, is what lies beneath the professional. It is a deep exploration of self and reflection on the people, places, and events that shape him. With this intimate and honest portrait, Dr. Smith takes us through the trials and tribulations of life, replete with the wisdom of experience and contemplation. What does it mean to live a life of value, of service?
Gratitude Four Years After Breast Cancer Surgery

"Entering the cancer world is scary and it takes a lot away from you..." On her breast cancer surgery anniversary, Emily was overcome with gratitude. She remembers all she endured, reflects on her life since, and gives thanks for her surgeon Dr. Roshni Rao, and the team who saved her life. Beautiful words from a persevering spirit.
Pancreatic Cancer Awareness Day, 18 Years Strong
Every year the experts at The Pancreas Center bring together the leaders in pancreatic cancer research and clinical care with patients and their families. It’s a day of community, celebration, and remembrance. This year brought presentations on the many transformative immunotherapy clinical trials underway, patient stories, and what to expect as artificial intelligence (AI) shows promise in screening for pancreatic cancer.
Cleft Lip and Palate Team Day Builds Community and Shares Joy
As Director of Cleft and Craniofacial Surgery, one of Dr. Thomas Imahiyerobo’s top goals is to break the negative social perceptions that surround those with cleft lip and palate and other craniofacial conditions. Cleft Lip and Palate Team Day serves that mission—every year patients, families, and friends come from near and far to share their stories and experiences and celebrate life. It’s always an event to remember.
Retirement of Transplant Pioneer Dr. Mark Hardy Shows How Far We’ve Come

After nearly 50 years of service, transplant surgeon Dr. Mark A. Hardy officially retired this year. Dr. Hardy played a crucial role in Columbia's history as one of the original founders of the Transplant Program at NewYork-Presbyterian Hospital/Columbia University Irving Medical Center. His framework for the program was based on the principle of combined clinical care between surgeons and nephrologists during a time when renal transplant programs were managed by one or the other discipline, never by both at once. This cooperation between disciplines led to major contributions in immunogenetics, immunosuppression, and treatment of autoimmune diseases and lymphoma.
Bringing General Surgery to a General Audience
Acute care surgeon Dr. Katherine Fischkoff has a keen interest in surgical education, medical ethics, and surgical quality. As the new Chief of the Division of General Surgery, her mission to better general surgery care expands from the OR and clinic to the online world of social media. Several weeks ago, Dr. Fischkoff made an educational video on Instagram about abdominal pain that reached thousands of viewers in 24 hours.
As we conclude 2023, we reflect on all we’ve accomplished and all there is still to do: furthering the mission that quality surgical care should be accessible, affordable, and within reach for everyone.
Best wishes to all this holiday season!


